 The Spetzler–Martin classification was grade 1. The lesion in the left upper cerebellar hemisphere was a nidus of the cerebellar AVM fed by the right PICA and the left superior cerebellar artery (SCA), draining to the transverse sinus through the tentorial sinus (Fig. While the left PICA was agenesis, the right PICA perfused the bilateral inferior cerebellar hemisphere (Fig. The DPICAAn was located in the telovelotonsillar segment of the right PICA. We performed digital subtraction angiography (DSA) to examine the DPICAAn and the possible nidus in the left cerebellar hemisphere. The lesion in the left cerebellar hemisphere revealed hypointensity on T2-star image, indicating past hemorrhage. A lesion, which was suspected to be a nidus of an AVM, was also detected in the left upper cerebellar hemisphere. Magnetic resonance imaging (MRI) revealed a right unruptured DPICAAn. Although no neurological deficit was apparent, a stroke event was suspected. The patient was a previous smoker and had a medical history of hypertension and dyslipidemia. The anatomical location of the DPICAAn and AVM contributed to the success of a single-session open surgery.Ī 67-year-old male presented with complaints of a headache. Open surgery can be considered for DPICAAn and cerebellar AVM. The cerebellar AVM was completely removed, and the DPICAAn was successfully clipped in a single-session open surgery. We selected open surgery to prevent any hemorrhagic event from the DPICAAn and the cerebellar AVM. The left PICA was agenesis, and the right PICA perfused the bilateral inferior cerebellar hemispheres thus, the right PICA could not be sacrificed. Magnetic resonance imaging raised suspicions of asymptomatic past hemorrhage in the cerebellar AVM.  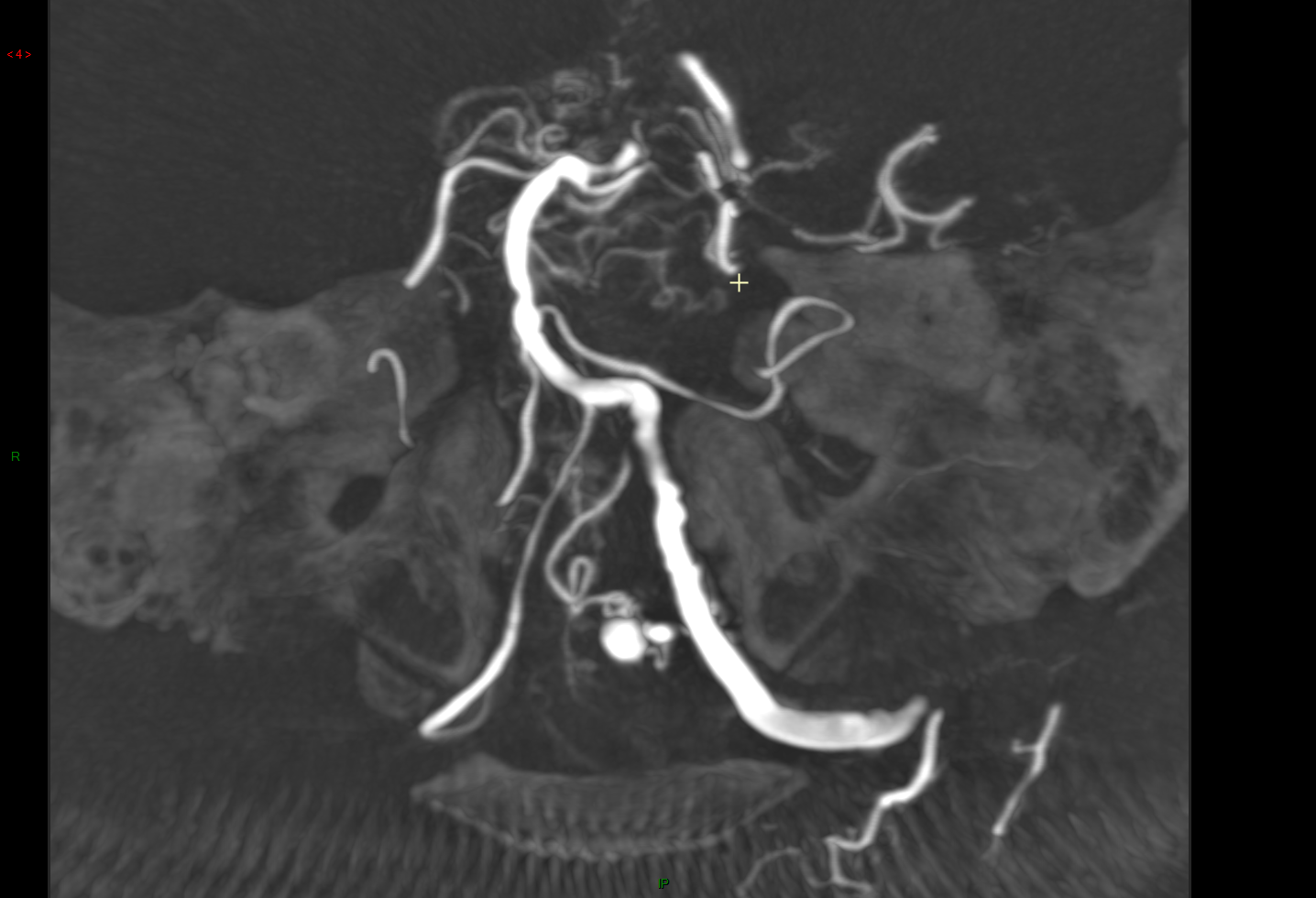
In addition, the nidus was located medially in the left upper cerebellar hemisphere. We detected a right DPICAAn in the telovelotonsillar segment and a cerebellar AVM primarily fed by the left superior cerebellar artery (SCA). Case descriptionĪ 67-year-old male presented with a headache. However, there have been few reports of simultaneous open surgery for coexistent cases of DPICAAn and cerebellar AVM. In previous reports about the treatment of a DPICAAn and a cerebellar AVM, endovascular embolization with the sacrifice of the posterior inferior cerebellar artery (PICA) has often been selected. The distal posterior inferior cerebellar artery aneurysm (DPICAAn) is reported to coexist or relate with the cerebellar AVM. The detection of a feeder aneurysm and an arteriovenous malformation (AVM) is relatively rare for the intracranial AVM. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
